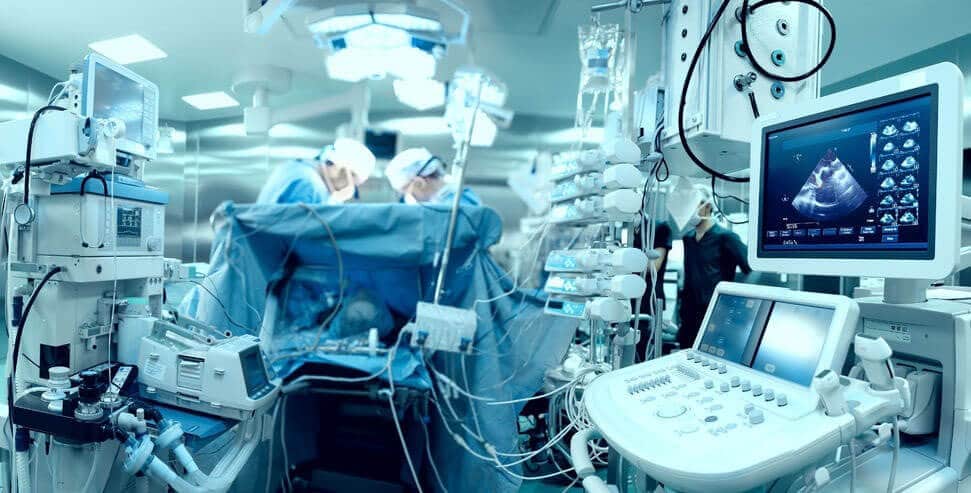
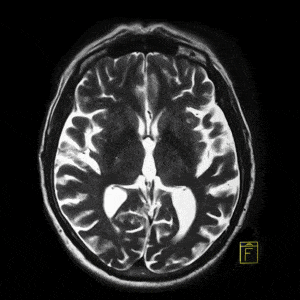
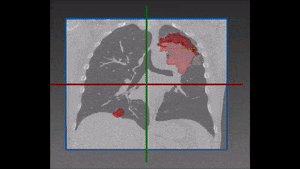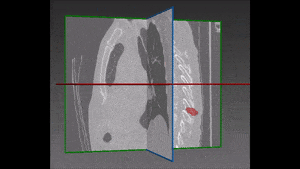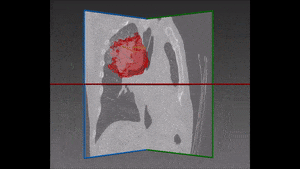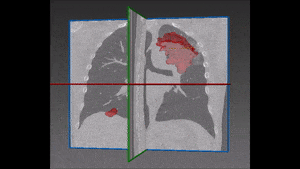
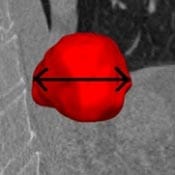
To construct a vision-aided catheter navigation system, the positions of blood vessels and segmented airways along the planned path of the catheter need to be accounted for. This allows to generate the shortest and safest catheter insertion trajectory, while allowing to plan the intentional puncture of non-critical tissues using the catheter, in order to arrive at a target site. Because CT scans are taken at static patient position, the real time imaging (fluorophore) needs to be registered with the airways and the vascular tree, and catheter position tracked over time. The irradiation dose needs to be reduced to non-damaging levels, resulting in poorly contrasted and noisy images of soft tissues. Recent developments in catheter hardware technology provide the means of acquiring additional local information based on MRI within vessels. Furthermore, sensors placed on catheter tips allow to detect whether the catheter is near lumen or vessel walls. This information can be integrated together to form a much clearer picture, while working almost blindly in a vessel which no endoscopic camera can have access to.
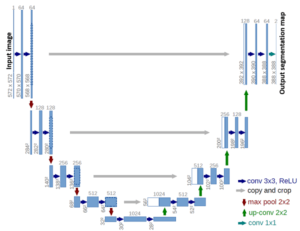
Path planning using the integrated sources of information (CT, airways segmentation and the like) can be done in several settings. A straightforward approach would be to utilize graph path techniques (e.g., Dijkstra, Bellman-Ford, etc.), where edges and nodes of the graph are defined by the architecture of the segmented vascular tree and the cost of the path is determined by measures of safety and other patient-specific physical constraints. This approach by itself, cannot account for off-vessel paths and therefore it needs to be reinforced by additional edges, which represent punctured paths. A complication arises when such paths are non-linear, and a tunnel needs to be dug inside a tissue. Hence, for this non-linear constraint it is most productive to work in the framework of machine learning.
Reinforcement Learning to support catheter navigation systems
Reinforcement Learning methods can be used to simulate the path taken by experts in a test setting, where negative rewards are given for dangerous paths and tunnels punctured. A combination of the graph optimization techniques, combined with Reinforcement learning for off-vessel planning, can provide the safest catheter trajectory path towards target. This and other highly complex algorithms are being constructed daily by the engineers of RSIP Vision. Our company is a global leader in constructing tailor-made computer vision, image processing and machine learning solutions for medical and other industrial domains. We have successfully done this for many years. Please use the contact page to consult our experts about your project. To learn more about RSIP Vision’s solutions and fields of expertise, please visit our projects page.